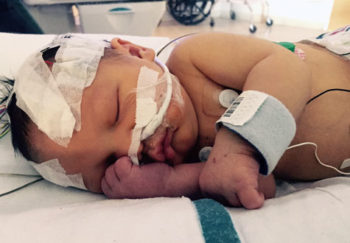
"You don't know how strong you are until you have to be," reflects Stephanie Nuckols on her baby Blaze's hearing loss and cochlear implants. "You don't know how strong your tiny babies are until they fight for their lives and, despite everything, make it through."
Blaze Ross was born with a twin. He and Gunner were both premature, 25 weeks early, with a host of complications. Both had brain bleeding that resulted in hydrocephalus, a build-up of fluid in the brain. But unlike Gunner, Blaze presented some additional complications.
Blaze had an opening between the heart vessels known as patent ductus arteriosus (PDA). And another complication would arise in the upcoming weeks: Blaze was failing his hearing tests.
New Hospital, New Discovery
It was a day Stephanie remembers as not only unexpected, but traumatic. The twins would need to be transferred to another hospital for surgery. The one place that had the technology to receive them was UVA.
When Stephanie and the twins arrived at UVA, she didn’t know what to expect. The NICU team at UVA provided the wide array of immediate, specialty care needed for Blaze and Gunner. “They were so amazing,” remembers Stephanie. “Although the experience was traumatic, the nurses, doctors and staff … I couldn’t have done it without (them).”
Providers told Stephanie to wait until they were home in hopes that continued hearing tests would screen differently. But this wasn’t the case. More hearing tests only confirmed her fears: Blaze was born deaf.
Choosing Cochlear Implants
For Stephanie, learning that Blaze was born without the ability to hear meant she had to make some difficult decisions about his life. She could either learn and teach Blaze and Gunner American sign language (ASL) or choose a cochlear implant procedure.
Stephanie was concerned about adding the challenge of learning ASL to the many trials Blaze was facing from a premature birth. Given everything, the choice of cochlear implants was a “no-brainer.”
Implant Surgery: An Outpatient Procedure
“Blaze’s hearing loss was severe enough to deem him a cochlear implant candidate,” explains speech pathologist Lori Bobsin, PhD, CCC-SLP, LSLS Cert. AVT. “We knew hearing aids probably would not work.”
A cochlear implant is an electronic device that helps those with severe hearing loss. A processor is placed behind the ear to transmit sound signals to a receiver under the skin behind the ear. The receiver sends the signals to electrodes in the inner ear, or cochlea. Surgery is necessary to implant these electrodes in the inner ear. From here, the hearing nerve is stimulated and the sound signals are sent to the brain.
“Cochlear implant surgery takes about two hours,” explains otologist Bradley Kesser, MD. “It’s an outpatient procedure, so the child comes to the hospital, has the surgery, and can go home the same day.”
Considering Cochlear Implants?
Find out if your child is eligible for implants and what to expect.
Speech Therapy: Catching Up to Gunner
"Blaze and Gunner are night and day," says Stephanie. "Both are sweet, loving and caring, but Blaze is my momma's boy, glued to my hip." She continues, "Gunner is up in your face, 'Give me your attention.' Blaze is more of a 'I like to play by myself' kind of baby, until he wants some love."
Having Gunner as a twin serves as a useful benchmark for Blaze's development in speech therapy.
"Our goal with his cochlear implants and with speech therapy is to have him catch up to his brother. Pretty much as soon as possible," says audiologist Cynthia Clark, AuD, CCC-A.
Bobsin adds, "If we get early intervention, if we have appropriate technology and qualified professionals and a parent who's motivated and dedicated, that child will develop to whatever level he would or she would have developed if she had not had a hearing loss."
Stephanie admits that therapy has not always been easy. "Therapy has been hard, to see some weeks with no progression."
"But he has come so far."
Watch Blaze's progression in the series below.
Cynthia Clark, AuD, CCC-A: I actually did Blaze's initial hearing screening when he was in the hospital in the NICU here at UVA.
Stephanie: When they told me that he had failed the screening test, I asked, I said, so what does that mean?
Bradley Kesser, MD: We don't know with 100% certainty why Blaze is deaf. But Blaze was born 25 weeks. He was born premature.
Lorin Bobsin, Ph.D., CCC-SLP, LSLS Cert. AVT: We have a pretty significant cochlear implant candidacy process because it's not an easy decision. We believe that they deserve to have resources. We believe that they need to have all the information to be able to make the decision that's right for their particular child. Blaze's hearing loss was severe enough to deem him a cochlear implant candidate because we knew hearing aids probably would not work for him.
Stephanie: Blaze is a twin, and we are a speaking family, so I feel like him not being able to hear us would alienate him.
Debbie Nuckols: They wanted us to try out the hearing aids. And then when we came back, discussed it, and then that's when it was just decided upon.
Kesser: Cochlear implants are one of the engineering marvels of the 21st and 20th century. The implant collects sound and turns that sound energy into an electrical signal. Cochlear implant surgery takes about two hours. It's an outpatient procedure, so the child comes to the hospital, has the surgery, and can go home the same day.
Stephanie: Which was surprising. I was under the impression that we were going to have to at least stay the night. He bounced back so fast, it was incredible.
Kesser: Once the bandage comes off, there is a small incision shaped like an "S" tucked in behind the ear and up into the hairline. About three to four weeks after surgery, the patient comes back to audiology for the activation of the cochlear implant. And if you've ever seen a cochlear implant activation, it is a very powerful and moving experience.
Stephanie Nuckols: It was incredible. He wasn't facing me, so I didn't get to see his initial reaction, but going back to seeing the videos that my mom took, it was what I expected.
Clark: It is a big day in the child and in the family's journey on this cochlear implantation.
Debbie Nuckols: When they turned them on, for a split second, it was stunned, and then it was crying.
Clark (off-screen): You know, he's hearing everything. And now, he's going to hear himself cry a little bit. What is that? I know. What was that?
[KNOCKING]
Clark: I hate to say that I like to see kids cry.
Stephanie: Right.
Clark: But this is good. He is hearing it. And he gave us some pretty good reactions to when we made a noise. He completely responded, which I think is awesome.
Stephanie: Yeah.
Clark: A lot of times, what happens is when the child is first turned on, they cry because they're scared because they're not used to hearing. Oftentimes it's a little bit startling. And for Blaze, that was definitely the case. But he calmed down pretty quickly after wearing them for only a few minutes.
Debbie: We want all the smiles and cooing. We did get that, but not right away.
Lorin Bobsin, Ph.D., CCC-SLP, LSLS Cert. AVT: Every time I talked, Blaze would turn and look to see who was talking. And it was really neat. It was an emotional time because he's now aware, and just 24 hours in.
Clark: Cochlear implants have to be quote unquote "mapped" or set for the recipient. So Blaze's cochlear-implant processor is going to be programmed differently than another child's cochlear-implant processor. And they're all different, and it's all individualized. So in the mapping appointments, we determine the level of stimulation that Blaze's auditory nerves need to process that sound and be stimulated by the implant.
Stephanie: So the next step is therapy. So we'll have therapy every week.
Clark: Blaze is really interesting because he has a twin brother who has normal hearing. And so to compare the two to each other, you might see a little bit of a difference right now. Our goal with his cochlear implants and with speech therapy is to have him catch up to his brother pretty much as soon as possible. And I think with a lot of hard work by Blaze's parents, and grandparents, and other caregivers, that, with his cochlear implants and with that hard work, we can have him catch up, and to have, essentially, the speech and language skills of his normal-hearing twin brother and his normal-hearing peers.
And many times in traditional speech therapy, the parents aren't involved. But in a listening and spoken language therapy session, the parents are in the room and actively involved. And it's mostly about working with the parents and giving the parents the skills they need to carry over the objectives once the family gets back home. In doing so, I try to tell families that if we get early intervention, if we have appropriate technology and qualified professionals and a parent who's motivated and dedicated, that child will develop to whatever level he would or she would have developed had she not had a hearing loss.
This past week we worked on body parts. So we talked about his eyes, and his nose, and his mouth, and his ears, and his belly. And we did a lot of work in looking in the mirror and not only having him identify these particular body parts on his favorite doll or his favorite bear, his favorite stuffed animal at home, but we also wanted him to be able to identify on his own.
He is an absolute joy to see in therapy because he hears everything, and he's understanding 15 or 20 words at this point at least. And he's saying eight or nine words at this point. And his mom always says, "He talks so much more at home than at therapy."
Yesterday during his session, we started singing the "Itsy Bitsy Spider." As soon as he heard it, even with mom not being in his sight, he put his fingers together to do the "Itsy Bitsy Spider." And I was like, he understands what that is.
Blaze Ross: I love you.
Stephanie Nuckols (off camera): I love you.
Blaze: I love you.
Stephanie: I love you.