This post was originally published in October 2017 and updated in April 2021.
Julia Martin recalls the day, 4 ½ years ago, when she went to go pick up her son, Conor, from his grandmother’s house. His grandmother said, “Conor told me he’s getting his new liver today.”
It was Julia’s birthday, so while that sounded like an amazing present, it also seemed unlikely. Conor, who was almost 3, had heard his parents talking about his potential liver transplant. It would treat his maple syrup urine disease. And it would give him a shot at a normal life without food restrictions or the risk of brain damage.
But they’d been waiting for two years, and so far, they hadn’t gotten a call that a liver was available. So Julia figured her son was just confused.
Right after she picked Conor up, they got the call. Conor was right. There was a liver waiting for him. The Martin family jumped in their car and made the 5-hour trip to UVA from their hometown of Stevens, Pennsylvania. A day later, Conor had his new liver.
A Split Liver Transplant & a Special Friendship
Conor’s family knows little about the donor. But they found a different connection through his new liver.
The day of Conor’s operation, surgeons did a left lateral segment transplant. During this, they split the liver into two pieces and gave the larger one to an adult. “This is important because it expands the donor pool and allows patients to be transplanted more quickly, and for more patients to benefit from transplant,” explains Frank DiPaola, MD, medical director of UVA’s pediatric liver transplant program.
While Conor was in surgery, Julia started chatting with another family in the hospital lobby. It turned out their loved one, 60-year-old Mike Honaker, was getting the other piece of the liver. For years, he had suffered from primary sclerosing cholangitis, a bile duct condition that leads to cirrhosis (liver scarring and damage). The transplant cured him, and he credits it with saving his life.
The day Mike left the hospital, he got to stop by Conor’s room and meet him. “He was quite shy,” Mike recalls. “I do a Donald Duck impersonation, and when I started talking to him like Donald Duck, his eyes got big, and he burst out in a smile.” Julia took a photo, and Mike later wrote “Big brother, little brother” on the back and framed it.
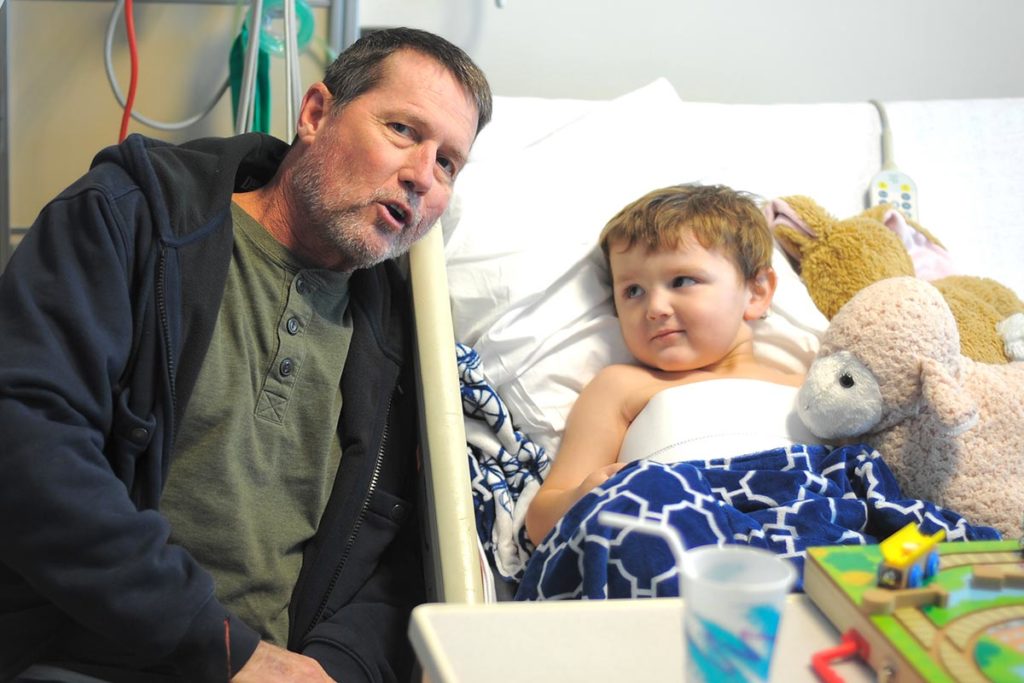
Since then, the families meet for lunch when their follow-up appointments in Charlottesville coincide, and Mike keeps up with Conor through Julia’s online updates. When Conor was sick several months ago, Mike led his church in prayer for him, with Julia joining through video chat.
4 Years Later: Complications but “No Regret”
Conor has had some post-transplant complications, including a bowel blockage and early-stage rejection. But he got through them with support from UVA Health Children’s, including the pediatric liver transplant team.
“We expect him to grow up with a healthy transplanted liver,” says DiPaola.
Before his transplant, most of Conor’s nutrition came from a formula. He could only have tiny amounts of protein because his body couldn’t process it.
“I can’t stress enough how strict it was,” Julia says. “Things that you don’t even think of as having protein — they do.” Conor threw tantrums because he couldn’t understand why he couldn’t eat the same food everyone else did.
Worse, even a simple cold or stomach virus could cause a buildup of proteins in Conor’s body, potentially triggering brain swelling, which could cause seizures and irreparable brain damage. Julia and her husband, Daryl, lived in fear of metabolic crises like this.
Now, that fear is gone. Conor eats a normal diet and loves brisket, pulled pork, eggs, and bacon — all things he couldn’t have before. He also enjoys sharing chocolates with his UVA nurses. “I save a lot for the nurses,” Conor says.
“I feel very positively about doing the transplant,” Julia says. “I have no regret. But when a child goes through all the things he’s been through, it’s difficult.”
Most recently, Conor had problems with narrowing of his bile duct, which carries secretions out of the liver. “This is the type of complication that a great transplant center needs to be able to recognize and manage,” DiPaola says.
A surgery team, including interventional radiologists and liver experts, did surgery to stretch Conor’s bile duct. The surgery was successful. Julia and Conor’s healthcare team are optimistic for his future health.
Growing Up After a Pediatric Liver Transplant
Conor takes everything in stride. He learned to take pills when he was two years old and now swallows his twice-daily handfuls without water. Because of monthly bloodwork, his transplant team catches problems early, so he usually doesn’t feel sick.
The child life team makes his hospital stays more fun — last year, they helped him build a volcano in his hospital room.
During his most recent stay, something even more exciting was in the works. The day after his discharge, Julia and Daryl adopted their fourth child, a 3-year-old girl named Caydence. Conor said, “We need to get home because I’m going to be a big brother.”

These days, Conor is enjoying life with his little sister, two older brothers, and parents. Although the Martins have largely spent the last year at home, Conor is attending in-person school. He wears a mask everywhere, and Julia says his school has played a big part in keeping him healthy.
Conor’s favorite class at school is “lunch,” and his favorite sports are basketball and fishing. On a recent trip with his brothers and dad, he caught a fish that was “about a foot long and weighs 3 pounds.”
He says he wants to be a doctor when he grows up. He's especially interested in ultrasounds and anatomy.
A Pediatric Liver Transplant Partnership
Pediatric Organ Transplants in Virginia
UVA performs pediatric liver, heart, and kidney transplants in kids of all ages.
Conor’s transplant was part of a then-new partnership with UPMC Children's Hospital of Pittsburgh to increase access to care for pediatric transplant patients. UVA Health Children's has now done 26 pediatric liver transplants as part of the partnership.
UPMC Children’s Hospital of Pittsburgh opened the country’s first comprehensive pediatric transplant center in 1981. The partnership allows patients and their families to go on both hospitals' transplant waiting lists, which can dramatically shorten the wait time for a new liver.
Watch Conor’s story from 2017 to learn more about his transplant and the partnership.



What a beautiful, wonderful story – is it possible to give us an update on Conor and his family in a few more months?