Angelo Dacus, MD, is upfront with his patient, Lisa Green.

“Most of the time these can heal with therapy, a splint, rest. “ He nods at her elbow, which she holds, in pain. “But most of the time, people don’t want to take the time.”
Dacus is talking about tennis elbow, or lateral epicondylitis, a condition that affects not just people who play tennis, but anyone who overuses their hand and wrist repetitively. Having been a rugby player, adventure racer, ultrarunner, and in general a physically active person for most of her life, Green’s elbow damage is not surprising. An MRI shows her ligament is torn and aggravated by a bone spur.
Green is nervous. Before Dacus arrived, she explained that she’s not the kind of person who likes to see doctors. She’s had surgery before, and it wasn’t a great experience – she had a reaction to the anaesthesia; the recovery was painful and long. She’s also afraid that, whatever the solution, she will be without her right arm for a long time. She’s right-handed. She doesn’t like to sit still.
Elbow Surgery vs. Physical Therapy
When Dacus arrived, the two discovered they both hail from Alabama and established a comfortable rapport. Green’s initial anxiety visibly subsides as Dacus addresses her situation.
“I see two main groups of people,” he explains. “Recreational sports and laborers. The sports people don’t want to stop playing, because that’s what they’re energetic about, and for the laborers, it’s a financial consideration—being out of work plus the cost of healthcare. But I’m pretty sure if we put your arm in a splint for six to eight weeks, your elbow will heal on its own. It’s just a question of whether you want to do that or not.”
“What about the bone spur?” Green asks. “Won’t that keep aggravating the joint?”
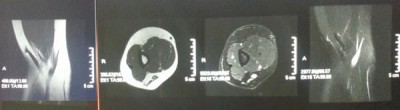
Bone spurs, Dacus explains, are more common than one might think. He suggests that, “looking at a sampling of patients over 40 would reveal a good 20 percent of them as having some bone spurs.” Dacus explains that wearing a cast to keep her wrist and arm from moving would allow the tissue to reconstruct on its own, bone spur or not. With just medication and physical therapy, it would take months, but could heal.
As Dacus outlines her options – waiting to see if the elbow will heal vs. surgery – Green listens, but shakes her head.
“I had surgery on my other elbow, and I don’t want to wait for this one to get worse like that one did,” she says. Green has already been wearing a wrist brace to help with her elbow and says, “I was immobilized, for weeks, then weeks of physical therapy, it got worse, and then I had to have surgery, more weeks of immobilization and weeks of therapy. So that could happen again, right?”
Dacus nods. “Yes.”
Green’s other worries: That she drives a stick shift, holds physically demanding jobs, has two school-age children, and there’s yard work and house projects she’s been waiting all winter to get to. Wearing a brace would prevent her from doing all of that—possibly with no recovery at all.
Dacus explains what surgery will entail and the recovery will involve. It’s an outpatient procedure, 45 minutes, followed by 10 days of rest, and six to eight weeks of therapy.
Green nods. “That’s not too bad.”
Dacus describes anesthesia options, and they settle on a nerve block.
The doctor examines her other elbow, and gently shows her where the surgery would occur, what the scar will look like, and he describes the layers of tendon in the elbow. Each layer pulls and moves the hand and wrist in different directions, and during surgery they will have to get to the one that is torn and do any reattaching necessary. During the procedure, Dacus will also shave away the bone spur.
Elbow Surgery: Scheduled
It’s not a short visit. A nurse checks vitals, another nurse goes over surgery preparation – screens Green for sleep apnea (see sidebar) – and a physician’s assistant (PA) goes over the details of the patient consent form necessary to authorize the operation. Even the scheduler reviews the pre-surgery procedure with Green after scheduling the date and time (which Green set around garden projects and vacation).
Sleep Apnea & Surgery
These days, healthcare providers must screen patients for sleep apnea before surgery. Sometimes, people are sent to do a sleep study to rule the disorder out. The reason? People with sleep apnea have more challenges with anesthesia. Know the symptoms of sleep apnea.
While all of this attention to detail not only helps to establish a roadmap of what to expect, the team’s coordination also calms Green’s nerves about surgery. She takes a deep breath. “I’m nervous,” she admits. “But it looks like I’ll be back in action by mid-June.”
As she is leaving, Green sees Dacus in the hallway. He confirms the date of surgery and jokes with her a little bit. “He’s a cool guy,” Green says. “I like him. You can’t go wrong with an Alabama boy.”
Is she happy with her decision to have surgery?
“Absolutely. I’m glad to get this done and have the pain fixed.”
Do You Have Joint Pain?
Visit the experts at the UVA Hand Center to discuss your options.

A 2014 reanimation of a dead post lol. Thank you for this article. it was helpful in considering my surgery. I have decided to go for it.